1 Centre de recherche du CHU de Québec-Université Laval, Regenerative Medicine Division (CRCHU), Department of Surgery, Faculty of Medicine, Université Laval and Centre de recherche en organogénèse expérimentale de l’Université Laval/LOEX, 1401 18ième Rue, Quebec, Quebec, G1J 1Z4, Canada
2 School of Physical and Occupational Therapy, McGill University, Centre de recherche du Centre hospitalier de l’Université de Montréal (CRCHUM), Hôpital de réadaptation Villa Medica, 225 Rue Sherbrooke E, Montreal, Quebec, H2X 1C9, Canada
3 Université de Montréal, Faculty of Medicine, Department of Surgery, Division of Plastic Surgery, 2900 Boulevard Edouard-Montpetit, Montreal, Quebec, H3T 1J4, Canada
4 CHU Sainte-Justine, 3175 Chemin de la Côte-Sainte-Catherine, Montreal, Quebec, H3T 1C5, Canada
5 Unité des Grands-Brûlés, Hôpital Hôtel-Dieu de Montréal, Centre Hospitalier Universitaire de Montréal (CHUM), 3840 Rue Saint-Urbain, Montreal, Quebec, H2W 1T6, Canada
6 Centre Hospitalier Universitaire (CHU) de Québec, Université Laval, 1401 18e Rue, Quebec, Quebec, G1J 1Z4, Canada
7 University McGill, Faculty of medicine, Department of Surgery, Division of Plastic Surgery, 3605 Rue de la Montagne, Montreal, Quebec, H3G 2M1, Canada
8 Centre of Genomics and Policy, McGill University, Faculty of Medicine, Department of Human Genetics, 740 Dr Penfield Avenue, Montreal, Quebec, H3A 0G1, Canada
9 Department of Molecular Biology, Medical Biochemistry and Pathology, Faculty of Medicine, Université Laval,1050 Avenue de la Médecine, Quebec, Quebec, G1V 0A6, Canada
§ These authors equally contributed to this paper
Abstract
Split-thickness skin autografts (AGs) are the standard surgical treatment for severe burn injuries. However, the treatment of patients with substantial skin loss is limited by the availability of donor sites for skin harvesting. As an alternative to skin autografts, our research group developed autologous self-assembled skin substitutes (SASSs), allowing the replacement of both dermis and epidermis in a single surgical procedure. The aim of the study was to assess the clinical outcome of the SASSs as a permanent coverage for full-thickness burn wounds. Patients were recruited through the Health Canada’s Special Access Program. SASSs were grafted on debrided full-thickness wounds according to similar protocols used for AGs. The graft-take and the persistence of the SASS epithelium over time were evaluated. 14 patients received surgical care with SASSs. The mean percentage of the SASS graft-take was 98 % (standard deviation = 5) at 5 to 7 d after surgery. SASS integrity persisted over time (average follow-up time: 3.2 years), without noticeable deficiency in epidermal regeneration. Assessment of scar quality (skin elasticity, erythema, thickness) was performed on a subset of patients. Non-homogeneous pigmentation was noticed in several patients. These results indicated that the SASS allowed the successful coverage of full-thickness burns given its high graft-take, aesthetic outcome equivalent to autografting and the promotion of long-term tissue regeneration. When skin donor sites are in short supply, SASSs could be a valuable alternative to treat patients with full-thickness burns covering more than 50 % of their total body surface area.
Graphical Abstract
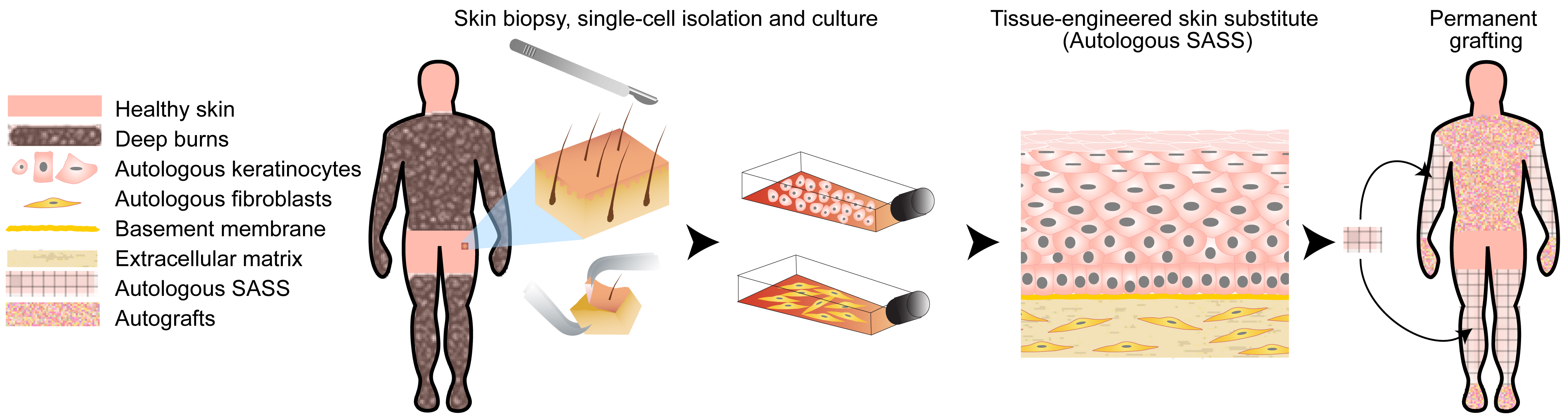
Keywords
- Autologous
- burn
- culture techniques
- connective tissue
- regenerative medicine
- skin
- skin grafts
- tissue culture
- tissue engineering
- tissue therapy
