Optimization of laboratory infrastructure and surgical workflow in preclinical rodent bone research: an underreported barrier to reproducibility
1 Institute of Metallic Biomaterials, Helmholtz-Zentrum Hereon, 21502 Geesthacht, Germany
2 Section Biomedical Imaging, Department of Radiology and Neuroradiology, University Medical Center Kiel, Kiel University, 24118 Kiel, Germany
3 Department of Functional Morphology and Biomechanics, Zoological Institute, Kiel University, 24118 Kiel, Germany
4 Chair of Functional Nanomaterials, Department of Materials Science, Faculty of Engineering, Kiel University, 24143 Kiel, Germany
5 Trauma and Orthopaedic Research Unit, School of Medicine and Psychology, John Curtin School of Medical Research, Australian National University, 2601 Canberra, ACT, Australia
6 Data-Driven Analysis and Design of Materials, Faculty of Mechanical Engineering and Marine Technologies, University of Rostock, 18059 Rostock, Germany
§These authors contributed equally.
Abstract
Preclinical surgical studies in rodent models play a pivotal role in elucidating the mechanisms of bone repair and regeneration. Similar to clinical practice, intraoperative and postoperative complications in preclinical studies significantly affect treatment outcomes and may even alter the overall experimental results. Well-established laboratory infrastructure and experimental procedures can reduce the risk of adverse events, such as intraoperative technical errors and postoperative infection. However, these aspects are often underreported or overlooked in the literature. In this study, fracture fixation in rats is presented as an example to highlight the essential but often unreported details, such as virtual surgical planning, preoperative rehearsal, disinfection protocols, intraoperative management, postoperative support, multidisciplinary collaboration, and research documentation. Supplementary and alternative solutions are also proposed for laboratories with limited resources. By applying virtual planning and rehearsal with three-dimensional (3D)-printed samples, the authors have performed 108 consecutive external fixation procedures for rat femoral fractures since 2020, with no intraoperative dropouts attributable to surgical technique errors. The operative time stabilized at 45.6 ± 3.8 minutes (mean ± standard deviation), reflecting low variability and a reproducible workflow. Systematic implementation of these strategies helps prevent postoperative complications, enhances animal welfare, and improves the reproducibility and translational potential of preclinical research.
Graphical Abstract
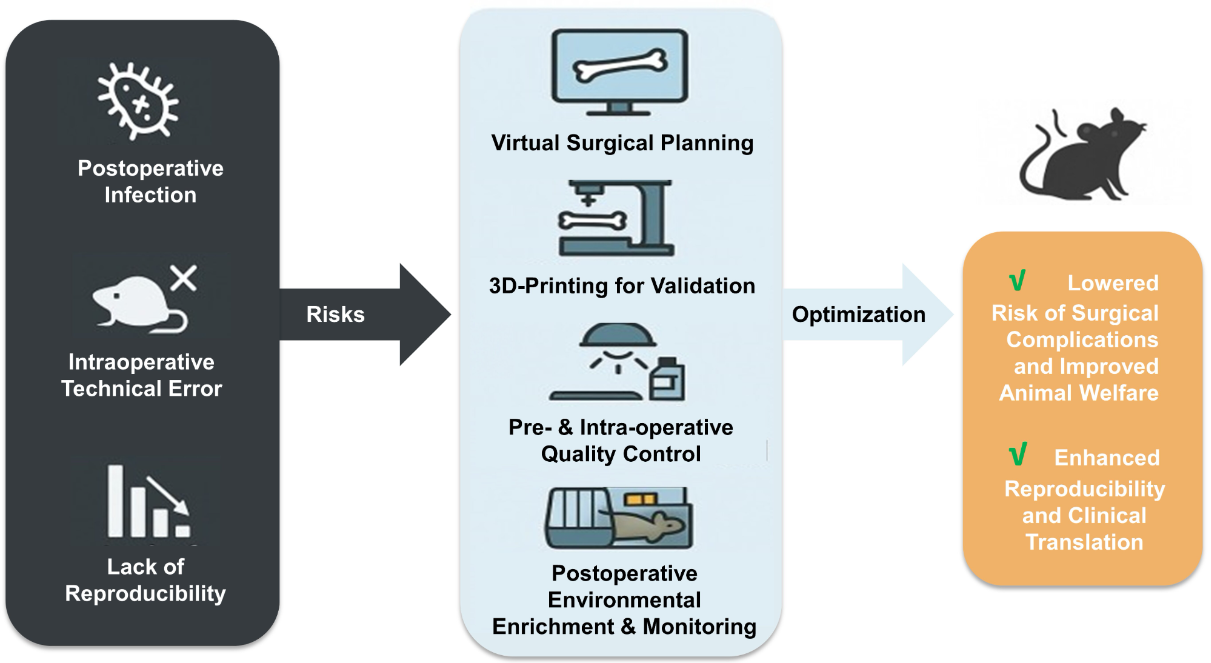
Keywords
- Orthopaedic procedures
- animal model
- three-dimensional printing
- infection control
- electronic lab notebook
- environmental enrichment
